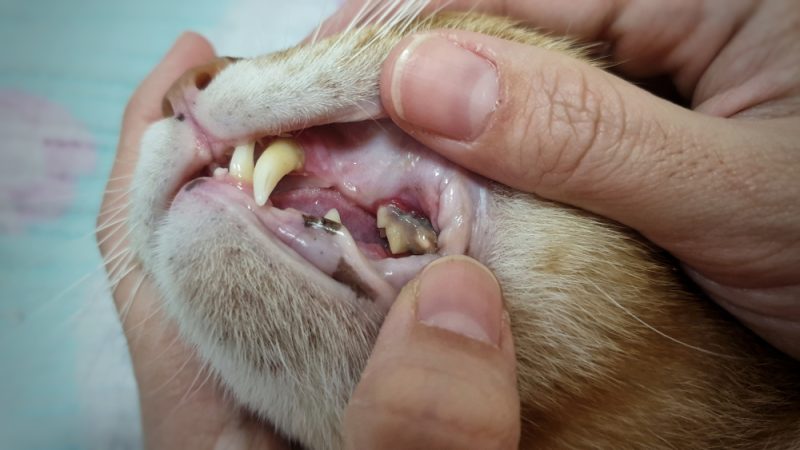
You may first notice bad breath, difficulty eating, or even bloody droplets in your cat’s food or water bowl. No matter how it initially crosses your radar, dental disease in felines is a big problem: It affects 50% to 90% of cats over 4 years old 1. The good news is that dental disease is completely preventable and in most cases, fully treatable. So, let’s look at the ins and outs of dental disease in cats.

What Is Dental Disease in Cats?
Dental disease is an all-encompassing term that refers to issues in a cat’s teeth and their related structures. While tooth problems may seem minor in the grand scheme of things, dental disease can contribute to problems in other areas of the body. When bacteria in the mouth get out of control, they can travel to other organs, potentially setting up life-threatening infections. The heart, liver, and kidneys are the main targets.
In other words, it’s important to get your cat’s oral health under control. The first step is knowing the signs.
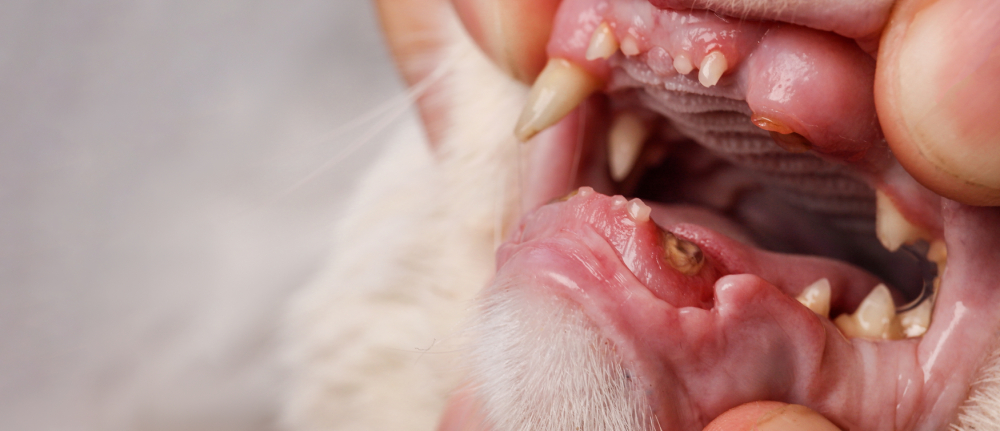
What Are the Signs of Dental Disease in Cats?
Kitties in the early stages of dental disease—which is the best time to treat it—may not show any signs. Instead, it’s usually diagnosed during a veterinary exam.
- Bad breath
- Pawing at the mouth
- Difficulty eating, especially hard kibble
- Head shaking and chattering jaws
- Drooling
- Bloody spots in the food or water bowl
- Decrease in appetite
- Weight loss
If you carefully lift your cat’s lips, you may see swollen and red gums, brown spots on the teeth, and maybe missing teeth.
Seek veterinary advice if you’re concerned about your pet’s well-being.
If you need to speak with a vet but can't get to one, head over to PangoVet. It's an online service where you can talk to a vet online and get the advice you need for your pet — all at an affordable price!
What Are the Causes of Dental Disease in Cats?
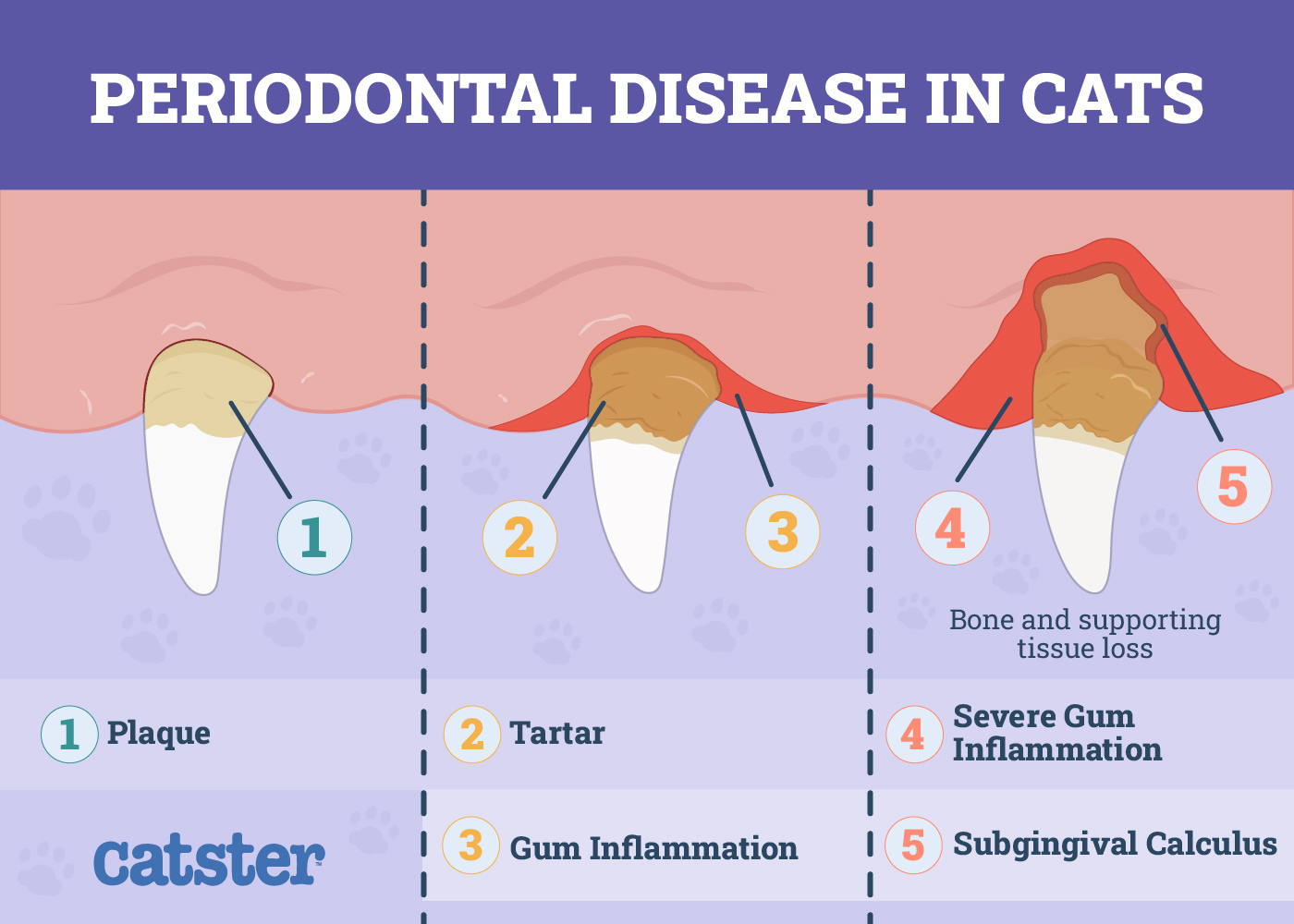
It all starts with the normal formation of plaque, which is a layer of beneficial bacteria that forms on the teeth. If it isn’t removed, the plaque hardens into tartar, which can be irritating and an excellent place for bad bacteria to gather. If plaque and tartar accumulations are significant enough or in nonpreferred areas, such as below the gumline or in between teeth, it can cause inflammation, pain, and even an infection. Here’s where the trouble starts.
- Gingivitis: This is when plaque and tartar sneak below the gum line, causing inflammation of the gingiva, or gums.
- Periodontitis: If gingivitis is left to its own devices, it can spread to the periodontal tissues, which are those that attach teeth to the jawbone. The inflammation can eventually weaken the tissues’ hold, creating loose or falling-out teeth.
- Tooth resorption: This is when the structures of the teeth start to break down, creating loose teeth and tooth loss. The exact cause of tooth resorption isn’t known.
Cats may also develop stomatitis, or inflammation of other parts of the mouth. This may be due to an over-the-top reaction to the buildup of bacteria or something unknown. Either way, stomatitis and other forms of dental disease can be uncomfortable, to say the least, making it so a cat doesn’t want to eat and otherwise decreasing their quality of life.
Gingivitis can also be brought on by other illnesses, such as kidney disease, viral infections, and diabetes. Regular veterinary care is the best way to check for and treat these illnesses.

How Do I Care for a Cat With Dental Disease?
Your kitty will thank you if you can catch dental disease before it becomes enough of an issue for them to start showing signs. The best way to do this is to see your veterinarian regularly. They will lift your cat’s lips and find any minor starts of dental disease before your cat has to show you themselves.
Otherwise, get a veterinary appointment as soon as you start noticing any of the signs. This will give your vet a chance to assess the progress and determine a treatment plan. Keep in mind that to get a good look inside your cat’s mouth, your vet may need to sedate them. They may also take X-rays to check on your cat’s jawbone and tooth roots. Fortunately, they can start treatment while your kitty is sleeping. This may include a thorough cleaning to remove plaque and tartar above and below the gumline. They can also extract any teeth that are loose or damaged. From there, depending on your cat’s list of issues, antibiotics and anti-inflammatories may be prescribed to treat further infections and inflammation.
Don’t try to remove tartar from your cat’s teeth on your own. Most cats don’t appreciate people messing around in their mouths, and they may resort to biting. Also, using tools to remove tartar can cause damage to your cat’s teeth or mouth. Instead, leave the work to your vet.

How Can Dental Disease in Cats Be Prevented?
Whether your cat has yet to experience it or they are currently recovering from a case of dental disease, there are things that you can do to prevent it. The best way to keep their teeth clean is exactly what you do: Brush them. It’s going to take a bit of training and coaxing, but most cats can learn to tolerate regular tooth brushings. Always use veterinary products, not human toothpastes, since some of the ingredients may be toxic.
The next step is to see your veterinarian at least annually for checkups and/or professional cleanings. If teeth brushing isn’t an option for you because you have a feisty cat, for example, ask your vet about the myriad dental care pet products that can help keep your cat’s teeth clean, such as gels, water additives, and tooth wipes. Just make sure to choose ones that are approved by the Veterinary Oral Health Council and your veterinarian.


Frequently Asked Questions
Can Cats Live With Dental Disease?
Dental disease isn’t necessarily a ticking time bomb, but it’s also not a pleasant experience for your cat. It can be painful enough to cause your cat to not eat. It can also create infections in other areas of the body, so it’s best to get your cat’s dental disease treated and under control as soon as you can.
How Fast Does Dental Disease Spread?
How quickly your cat goes from a clean mouth to loose and falling-out teeth will depend on the exact issue. Dental disease is progressive if left untreated, but that progression can be affected by several factors, including your cat’s overall health and the type of food that they’re eating.
That said, plaque usually takes 12–24 hours to turn to tartar, so daily tooth brushing can help significantly delay the progression of dental disease by preventing plaque formation.

Conclusion
Dental disease is a common issue found in cats, but it’s fortunately preventable. Be sure to see your veterinarian for regular oral exams and professional cleanings as needed. At home, regular tooth brushing or administrating other dental care products can help prevent dental disease and the associated pain and discomfort.
Featured Image Credit: RJ22, Shutterstock