In this article
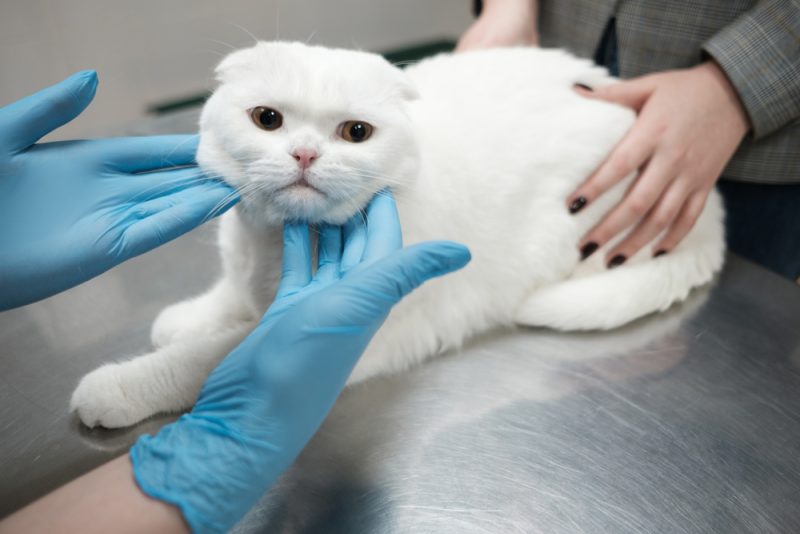
View 5 More +Feline orofacial pain syndrome is a chronic disease that affects cats. It is characterized by sudden onset, severe facial and oral pain. Affected cats may mutilate their own faces and the insides of their mouth. They often present with signs of excessive licking and exaggerated chomping and chewing movements. If not addressed, cats can cause considerable damage to their face and mouth, and it can be extremely distressing.
It can occur in any cat; however, Burmese cats seem to have a genetic predisposition for the syndrome. The syndrome is believed to be a chronic neuropathic pain disorder. There is no cure, but there are a few different management options that are focused on controlling the pain. It is a debilitating disease that causes a lot of distress and discomfort.

What Is Feline Orofacial Pain Syndrome?
Feline orofacial pain syndrome is a relatively rare disease seen in cats. Owners report their cats start to mutilate their faces and the inside of their mouths in an aggressive manner. The behavior seems to be linked to acute, severe pain in this area. The pain and discomfort witnessed are usually reported to be a more violent reaction than expected for a painful issue in this area.
In most cases, there does not seem to be a logical explanation for the pain reaction, therefore it is believed to be neuropathic pain. Cats will often have exaggerated chewing and licking behaviors as well as pawing at their mouths. The disorder has been compared to trigeminal neuralgia in people. The duration of an episode can last a few minutes or several hours therefore cats can come to a substantial amount of harm during this time.
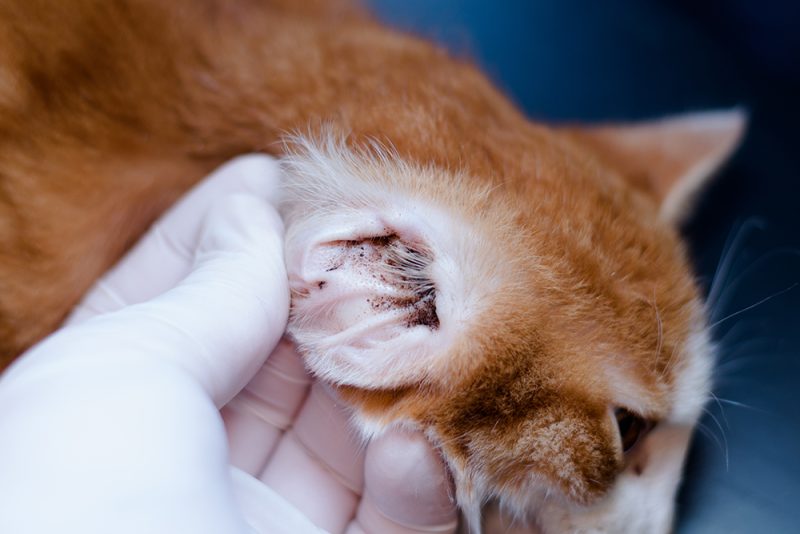
Often cats present with the problem on just one side of their face. The pain reaction typically comes in waves although some cats appear to experience continuous discomfort. There are triggers such as eating, drinking, or grooming—when the cat uses their tongue frequently. Dental disease and stress are also believed to contribute to the development of episodes. Cats can often go off their food and refuse to drink as they associate these activities with the pain.
Burmese cats are often affected, although it has been reported in other breeds such as Siamese and Tonkinese. This leads us to believe it is a condition that is inherited.

What Are the Signs of Feline Orofacial Pain Syndrome?
- Excessive licking
- Exaggerated chewing motions
- Self-induced trauma to the face and oral cavity
- Frequent pawing at the mouth
- Typically, clinical signs are one-sided
- Off food/unable to eat (in some cases)
Other characteristics that are sometimes surprising are that there are no neurological deficits, and the trigeminal nerve has no motor or sensory issues. The pain is always localized to the lips and mouth, nowhere else around the face seems to be affected.
Typically, it only affects one side of the face.

What Are the Causes of Feline Orofacial Pain Syndrome?
The exact cause of feline orofacial pain syndrome is not currently known. More research is required on this subject. It is thought to be due to abnormal interpretation of pain messages by the nervous system and is called a neuropathic pain disorder. It has been compared to trigeminal neuralgia in people. Here a pain sensation is brought about by dysfunction or damage of the trigeminal nerve which supplies sensation to the mouth and face area.
It is believed that cats suffering from this condition experience a misfiring of the trigeminal nerve. It is thought that neuropathic pain conditions can be exacerbated by internal and external factors such as stress.
Cats with feline orofacial pain syndrome are often reported to be cats that will become stressed by other animals in their household or in their neighborhood (if they are outdoor cats). They may also get very stressed when taken to a cattery or the vet. It is important that owners are aware of potential triggers to avoid cats causing themselves a great deal of damage.
There are thought to be some factors that seem to trigger episodes or contribute to the development of the disease.
- Injury to the face and/or mouth
- Nutritional deficiencies
- Dental disease
- Stomatitis
- Gingivitis
- Viral infections
- Genetics

Diagnosis of Feline Orofacial Pain Syndrome
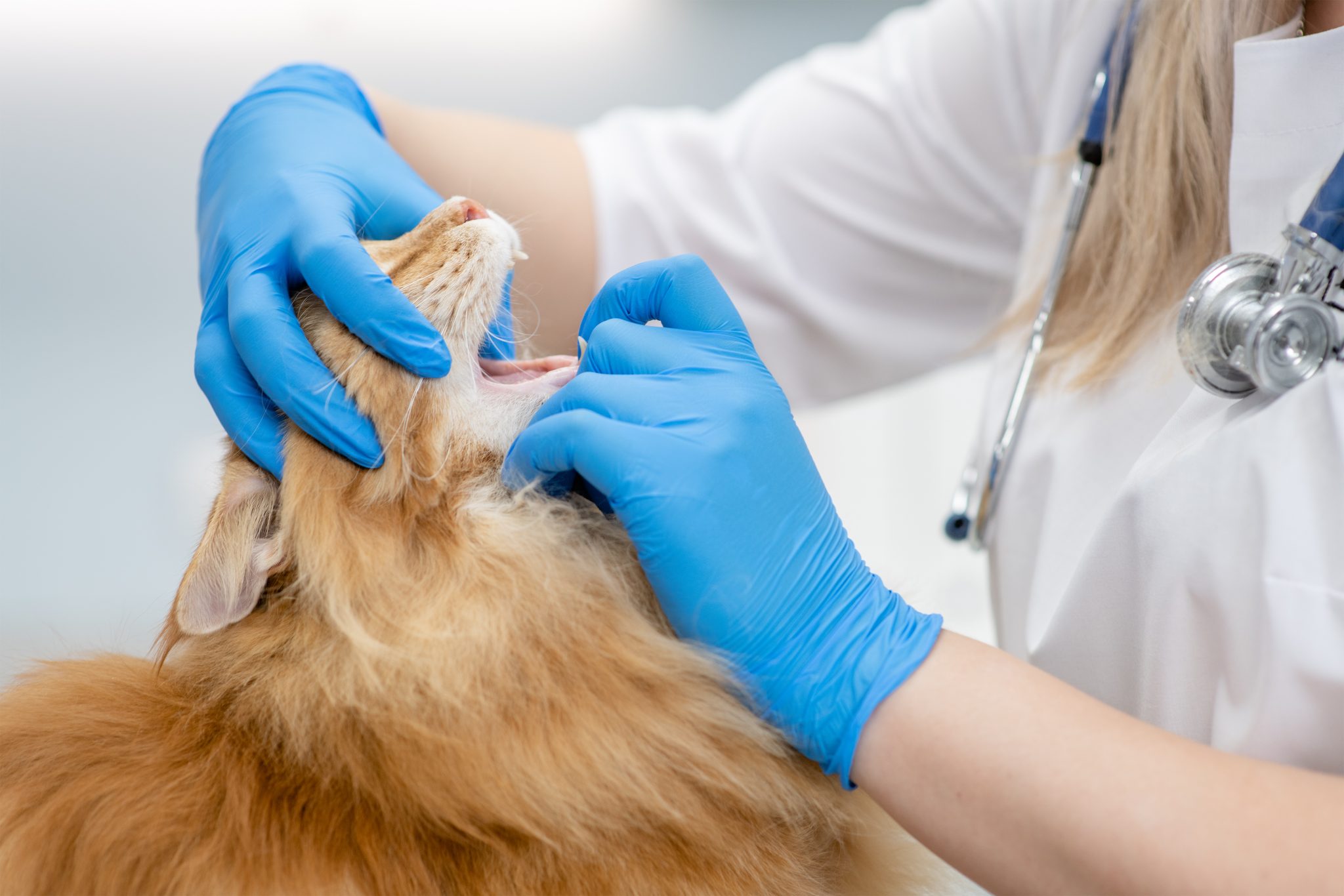
A vet will take a full clinical history from you and perform a physical exam. It will be very useful if you have any videos of your cat showing any clinical signs as they may not show any signs at the vet’s. The vet will attempt to examine your cat’s mouth if they will tolerate it.
They may want to take blood tests and a urine sample to rule out other diseases that may cause similar signs. Diagnostic imaging such as X-rays and ultrasound can be helpful to rule out other diseases too such as tumors and dental problems. There is no specific test for feline orofacial pain syndrome, diagnosis is based on history, and clinical signs along with the absence of other diseases that cause similar clinical signs.
How Do I Care for a Cat with Feline Orofacial Pain Syndrome?
There is currently no cure for feline orofacial pain syndrome. Treatment aims to prevent self-mutilation and manage the pain experienced.
- Pain relief: Depending on the severity of the case this can be non-steroidal anti-inflammatories on their own or other stronger painkillers such as opioids.
- Anticonvulsants: Medications such as gabapentin can be used. Gabapentin is thought to be useful in the treatment of neuropathic pain as it modulates nerve signals, therefore reducing the perception of pain.
- Antibiotics: These may be indicated if the injuries to the face lead to a bacterial infection.
Consulting a veterinarian is recommended for the best course of action.
If you need to speak with a vet but can't get to one, head over to PangoVet. It's an online service where you can talk to a vet online and get the advice you need for your pet — all at an affordable price!

The vet may recommend behavioral training to attempt to address triggers that can be controlled. Some cats will respond well to environmental enrichment toys to distract them. This is not suitable for all cats, as for some, this exacerbates the condition as they become triggered when they chew on the toys. It can be difficult to find out what suits your cat. It is very important to be mindful of potential stressors in your cat’s environment and try to create a calm and stress-free environment wherever possible.
Some vets will advocate the use of an Elizabethan collar (a cone) over your cat’s head to prevent them from self-mutilating. This is useful as it prevents your cat from causing harm to themselves. This is not a suitable option to use alone, as your cat will still be experiencing the perceived pain. Preventing them from hurting themselves is very helpful, however they will still be suffering unless the pain is managed somehow.
In very severe cases, sometimes surgery is indicated. This can include dental procedures if the cat has dental disease present. Sometimes the damage sustained from self-mutilation requires surgical repair such as lip lacerations or damage to the tongue.


Frequently Asked Questions
What is the prognosis for a cat with feline orofacial pain syndrome?
If early diagnosis is made and treatment is given promptly, many cats go on to live a relatively comfortable life. Controlling the pain is the most important thing and if this is not achieved, the cat may end up suffering unduly.
Should I breed from a cat with feline orofacial pain syndrome?
Feline orofacial pain syndrome is thought to be inherited, although more research is required to confirm this. If this is the case, it would be frowned upon to breed from cats with the syndrome as they would be likely to pass it on to their offspring. This can be difficult to manage as the clinical signs of the syndrome may not become apparent until much later in the cat’s life after they have been bred.
Can I prevent feline orofacial pain syndrome?
It is not possible to prevent the syndrome although there are some measures owners can take to reduce the incidence of episodes in some cases. As environmental factors such as stress and dental disease can trigger episodes, it is advised to keep up with your cat’s oral hygiene practices and attend a vet regularly for dental checkups.
Where at all possible, reduce stress or remove potential stressors from your cat’s environment.

Conclusion
Feline orofacial pain syndrome is a disease characterized by episodes of severe oral and facial pain. Cats will mutilate themselves in an attempt to relieve the pain they experience. It can be extremely distressing for both cats and owners.
It is thought that lesions in the mouth (such as those caused by dental disease) and also stress can trigger episodes. The disease is believed to be a neuropathic pain disorder that is similar to trigeminal neuralgia in humans.
Treatment options are focused on controlling the pain to reduce the clinical signs. Supportive care is also necessary as quite often there are substantial wounds that need addressing.
If you think your cat may have feline orofacial pain syndrome, contact a vet immediately.
Featured Image Credit: MakeStory Studio, Shutterstock