For reasons unknown, cats may develop a painful inflammatory condition in their mouth. This is called stomatitis and may be the result of an overactive immune response to plaque and bacteria in the oral cavity. The typical treatment is to surgically remove some or all of the teeth to decrease the number of surfaces that bacteria can adhere to. Most cats do quite well after the recovery process, with a notable increase in their comfort level.

What Is Stomatitis in Cats?
In medical terminology, the prefix stomat– means mouth, and the suffix –itis means inflammation. Together, these combined words mean “inflammation of the mouth.” Affecting up to 10% of cats, stomatitis is a painful disease involving the gums, tongue, mucous membranes of the oral cavity, and in some cases, the back of the throat1. You may also see feline stomatitis referred to as feline chronic gingivo-stomatitis.
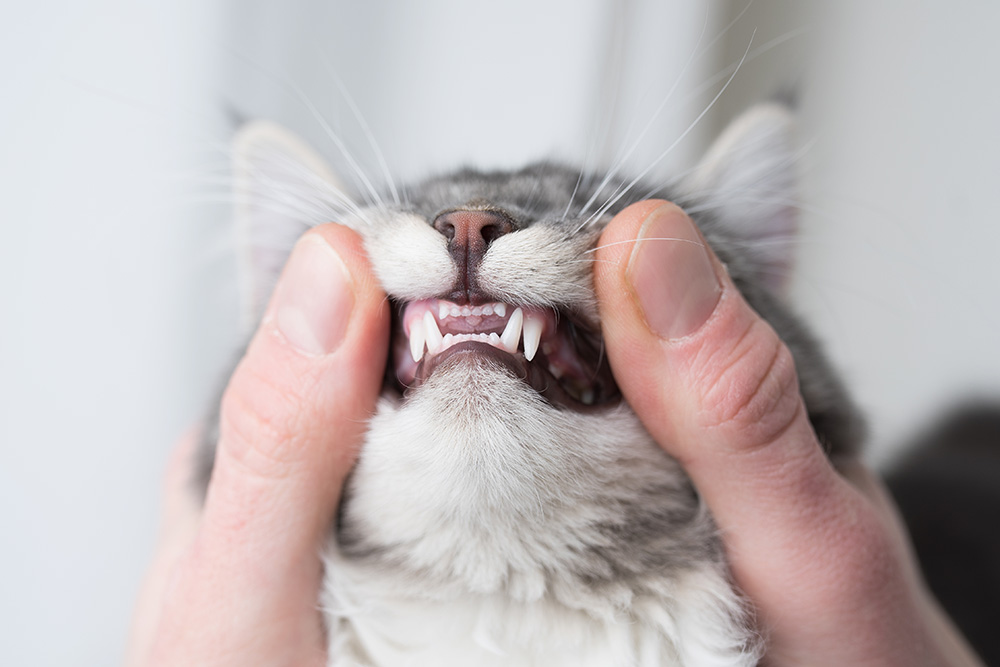
What Are the Signs of Stomatitis in Cats?
In general, signs of stomatitis may include:
- Bad breath
- Drooling
- Lack of grooming
- Dropping food
- Crying out in pain when eating
- Inappetence
- Weight loss
- Reluctance to yawn
If your pet is showing these signs, we suggest you speak to a vet.
If you need to speak with a vet but can't get to one, head over to PangoVet. It's an online service where you can talk to a vet online and get the advice you need for your pet — all at an affordable price!

What Are the Causes of Stomatitis in Cats?
Unfortunately, the causes of this painful and progressive disease remain unknown. It seems to be an underlying abnormality in the cat’s immune response or a heightened immune response to plaque and bacteria on the teeth, but this has not been confirmed. Viruses like feline immunodeficiency virus and feline leukemia virus may also play a role in the development of stomatitis.
How Is Stomatitis in Cats Diagnosed?
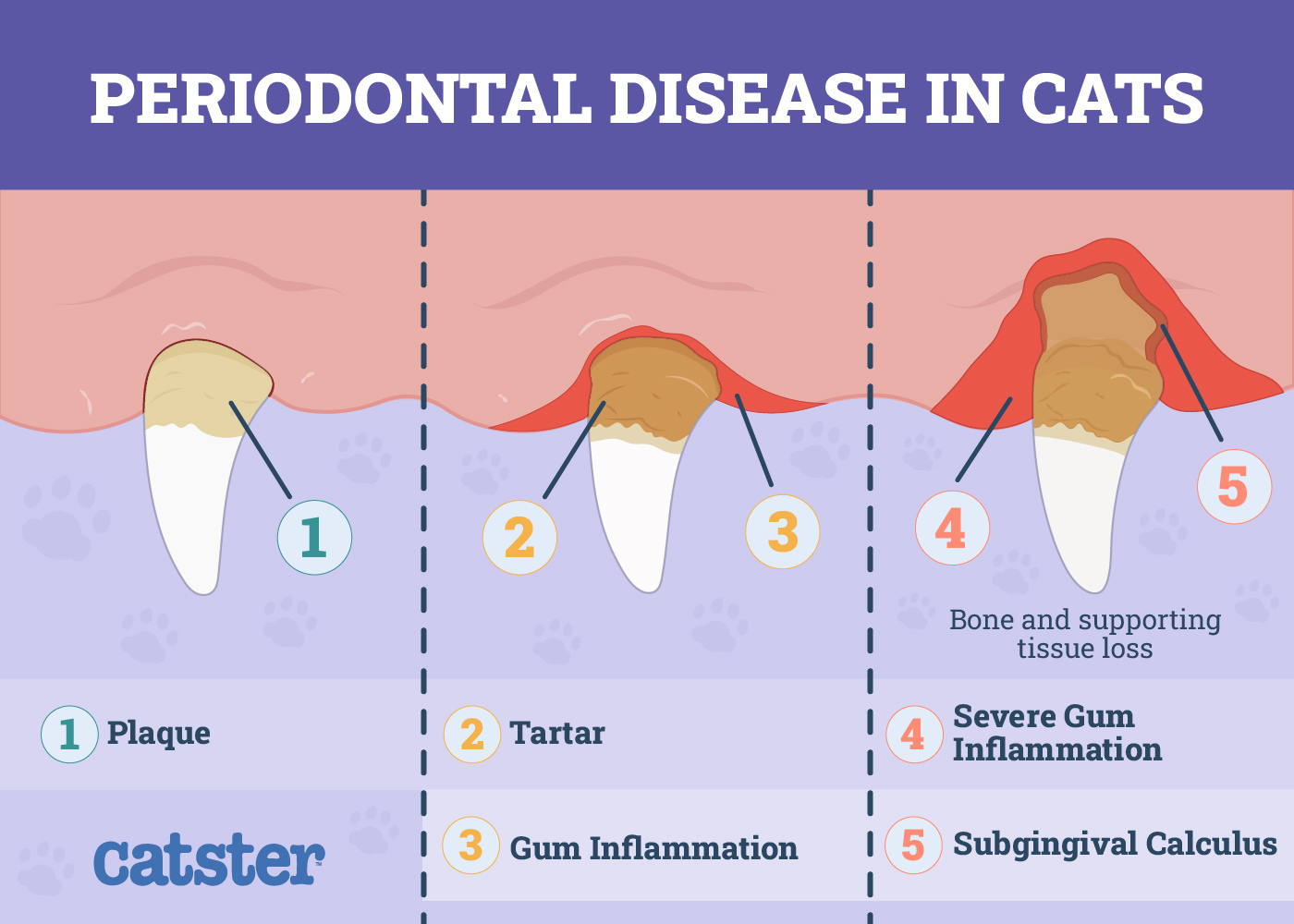
Your veterinarian may diagnose stomatitis after performing a thorough examination of your cat’s mouth. Findings may include substantial inflammation and redness of the gums, inside of the cheeks, and the back of the mouth. It is not uncommon for cats to also have periodontal disease and tooth resorption in conjunction with stomatitis.
How Do I Care for a Cat With Stomatitis?
Currently, the best way to treat stomatitis in cats is by surgically removing the teeth. This is done to reduce the oral bacteria and plaque that may be causing an inflammatory response. Approximately 90% of cats diagnosed with stomatitis that have undergone partial or full-mouth tooth extractions have resolved all signs of pain and inflammation, thus increasing their comfort and well-being. Your veterinarian may refer you to a veterinary dentist to perform the specialized surgery.
If your cat normally eats hard kibble, transitioning them to a moist or softened food diet (i.e., canned food) before surgery can help the recovery process, as cats must typically remain on a softened diet for 2–3 weeks after surgery. Your veterinarian will also provide at-home medications to lessen the pain and inflammation during healing. If your cat is reluctant to eat, a medication to stimulate your cat’s appetite may also be prescribed. Once your cat is completely healed, they may transition back to a hard kibble diet if they are willing to eat it.

Frequently Asked Questions
Is Stomatitis Curable?
The current recommendation is to perform partial or full-mouth tooth extractions to resolve the inflammation and pain.
Is Stomatitis Contagious to Other Cats?
No, stomatitis is not contagious. It cannot be passed from one cat to another.
Will My Cat Be Able to Eat Without Any Teeth?
Yes, most cats adapt quite well to having no teeth. In fact, you will likely see improvements in your cat’s quality of life and well-being once the pain and inflammation are gone.

Conclusion
Stomatitis is a painful condition in cats that affects the gums and soft tissues of the mouth. Causes remain unknown but may be related to an abnormal immune response to plaque and bacteria. Signs may include bad breath, difficulty eating, drooling, and weight loss. Current treatment recommendations include partial or full-mouth tooth extractions to resolve the pain and inflammation. Most cats do well after surgery, with an increase in comfort and well-being.
Featured Image Credit: Elena Kutepova, Shutterstock