In this article
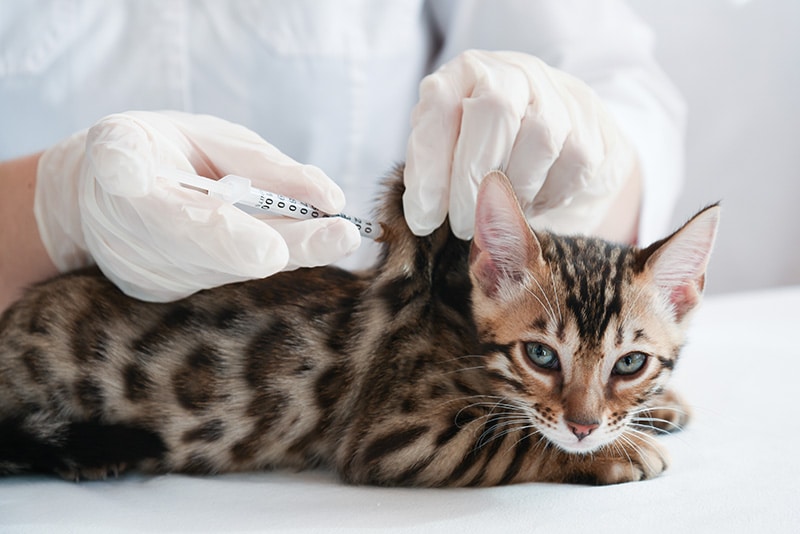
Injection-site sarcomas, also called feline injection-site sarcomas (FISS), are cancerous skin tumors that can develop in cats after they have received an injection, more specifically a rabies or leukemia vaccine 1. This is an uncommon but serious adverse reaction that can develop in one in 1 to 10 of every 10,000 vaccinated cats , sometimes years after a vaccination. The exact way in which these vaccines cause sarcomas is still unknown, but the most widely accepted hypothesis is that a local post-vaccination (or injection) inflammatory process leads to tumor growth.
It is important to understand that although this condition appears to be linked to vaccines, the benefits of vaccination still outweigh the risk of a cat getting a FISS post-vaccination. That is why it is strongly recommended to discuss any concerns that you may have regarding this topic with your veterinarian.
Here, we discuss important facts about injection-side sarcomas that every cat parent should know.

Important Definitions
Here are two important terms that you’ll see throughout the article.
Vaccination
The first time the immune system encounters an infection, it takes a while to mount a defense. It starts with a generalized inflammatory response, and over time, the immune system ‘learns’ to target the infection more specifically.
Vaccination works by introducing a killed, modified or mutated version of a virus into the body. The immune system reacts to the virus, creating memory cells, which will respond and replicate more quickly and efficiently the next time that virus is encountered. The form of the virus used in vaccination is either only able to replicate minimally, or not at all.
Adjuvanted Vaccine
An adjuvant, such as aluminum salts, is a substance that is added to vaccines to make them more effective by strengthening the body’s reaction to them. It causes a bit of inflammation at the injection site, which is necessary for the body to produce an immune response. But this inflammation can sometimes cause side effects.
According to the CDC, adjuvanted vaccines tend to cause more adverse reactions, such as redness, swelling, pain, fever, chills, and body aches, than non-adjuvanted vaccines.

Non-adjuvanted Vaccine
Non-adjuvanted vaccines, also called recombinant vaccines, use a modified viral agent to carry the DNA of the target virus, which replicates briefly within the host, resulting in a rapid immune response 2. Essentially, DNA from the virus being vaccinated against is ‘smuggled’ into the body inside a non-feline virus. Because of the nature of the viral vector, it triggers a rapid response, but the immune system quickly stops it from replicating.
Currently, the only available recombinant vaccines for cats in North America are vectored vaccines, which use a canarypox virus as a vector. Vectored vaccines using canarypox don’t need adjuvants, and they’re linked to a lower risk of injection-site sarcomas in cats. The trade-off is a much shorter period of immunity than with adjuvanted vaccines.

The 9 Important Facts About Injection-Site Sarcoma
1. Injection-Site Sarcomas First Appeared in 1991
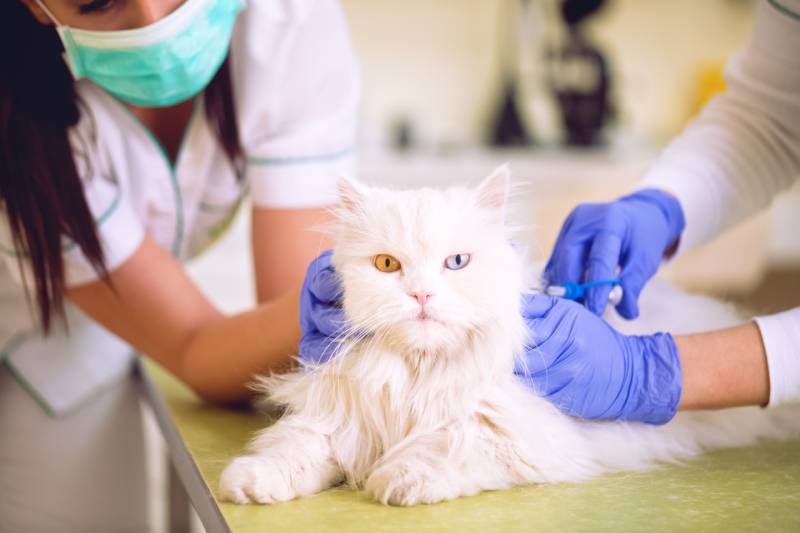
The first reports of these aggressive skin tumors emerged in the United States in 1991, and were subsequently reported throughout North America and Europe. However, this disease remained something of a mystery for more than a decade. According to a Canadian study that looked at 11,609 feline skin mass submissions from 1992 to 2010, the challenge in describing these tumors was mainly linked to:
- Poor vaccination records
- Limited long-term clinical follow-up information
- Refusal of vaccine manufacturers to disclose proprietary information about vaccine formulation
2. Injection-Site Sarcomas Are the Most Serious Side Effects Following Vaccination
In cats, the most serious adverse effect following vaccination is the appearance of these cancerous skin tumors (mainly fibrosarcomas), which develop under the skin at the sites of vaccination or previous injection. They behave more aggressively than other types of skin tumors, and can spread quickly throughout the cat’s body (metastasize), even after surgery. The rate of metastasis ranges from 10% to 28%.
3. The Exact Cause of Injection-Site Sarcomas Is Still Unknown
While a specific cause has not yet been identified, it is generally agreed that the inflammatory response triggered by the administration of injectable products (such as vaccines) contributes to the development of sarcomas in cats. However, the exact role of adjuvants, including those containing aluminum, in the pathogenesis of FISS are not fully understood.
Many believe that vaccines that use adjuvants, which have a higher incidence of localized and systemic inflammatory side effects, are most likely to be associated with FISS, with rabies and leukemia vaccines being the most prevalent. However, as cats often receive more than one vaccine at a time, and in their lifetime, a definitive cause is yet to be determined.
4. Injection-Site Sarcomas Can Be Diagnosed Years After Vaccination
The interval between vaccine administration and detection of sarcoma in cats has been known to range from 4 months to 15 years. However, the average is 1 to 3 years. Moreover, this long interval leads to even more confusion in finding the real culprit, i.e., which product and which vaccine may cause the sarcoma.
5. Injection-Site Sarcomas Have a Low Prevalence
According to the American Veterinary Medical Association, FISS are considered rare. Studies do vary in their reported incidence rates, from as low as 0.003 to 0.1% of vaccinated cats.
6. Injection-Site Sarcomas Have a High Risk of Recurrence
Injection-site sarcomas are invasive, meaning they have an extremely high risk of returning after surgery. The chance of cancer spreading increases the longer the cat lives, even if the tumor is removed completely.
This might happen for the following reasons:
- Cats receiving aggressive treatment (such as radical excision, radiation, and chemotherapy) survive longer and are more likely to have metastatic disease.
- Some treatments may directly promote metastases.
7. There Have Been Changes in Vaccination Protocols Since 1996
Following the report of the first cases in 1991, there have been changes in vaccination guidelines in North America, such as:
- More selective use of leukemia vaccination
- Less frequent vaccination for rabies
- Vaccination sites being more amenable to amputation (eg. over a limb instead of in the scruff)
- Introduction of non-adjuvanted rabies and leukemia vaccines (PUREVAX) in 2000
8. Injection-Site Sarcomas Can Occur in Various Locations
According to a 2017 study analyzing 392 post-vaccinal sarcoma cases in the US from 1990 to 2006, there has been a significant shift in their location due to changes in vaccination practices.
Before 1996, most of these sarcomas were in the interscapular regions, with tumors occurring there five times more frequently than on any other part of the cat’s body. This was typical because vaccines were often administered in the interscapular region.
However, following the vaccination protocol changes in 1996, the pattern shifted. Post-1996, these tumors are more commonly found on the hind legs.

9. Other, “Safer” Vaccines Are Available But Have Drawbacks
Non-adjuvanted rabies and leukemia vaccines exist, such as PUREVAX. These are considered “safer” because their reduced inflammatory response is associated with lower rates of malignant tumors.
However, these vaccines have two major downsides compared to the adjuvant vaccines:
- They are more expensive.
- They are approved for use as annual vaccines*
In comparison, traditional adjuvanted vaccines are generally more economical, and only need to be given every 3 to 4 years. Therefore, the schedule for adjuvanted vaccines is more aligned with the current recommendation for rabies and leukemia vaccines, which is to vaccinate “only as often as necessary.”
- Note on the PUREVAX non-adjuvanted rabies vaccine: The European Medicines Agency states in the product information that PUREVAX can be administered 1 year after the primary vaccination and then at intervals of up to 3 years.

Should You Still Vaccinate Your Cat?
The decision of whether or not to vaccinate your cat must be between you and your vet, unless you are traveling outside the US and are required to vaccinate your cat for travel. Knowing that there is a potentially fatal tumor associated with vaccination, this decision can often be difficult to make, and some statistics can be helpful to know.
If you need to speak with a vet but can't get to one, head over to PangoVet. It's an online service where you can talk to a vet online and get the advice you need for your pet — all at an affordable price!
- The prevalence of feline injection site sarcoma is between 0.003 and 0.1% of vaccinated cats.
- Feline leukemia is the most common infectious cause of disease in cats worldwide, for which there is no cure.
- The prevalence of feline leukemia in the US is approximately 3.1%.
- Rabies is present throughout the US, and is invariably fatal in pets.
- Both rabies and leukemia require close contact with infected animals, so risks are significantly reduced/eliminated in cats kept exclusively indoors.
- Cats can be tested for leukemia virus to minimize the risks from any new additions to your household.
All vaccines carry risks, but those risks are typically much less common than the diseases they prevent. It is important to assess the risks and benefits of vaccinating against certain diseases, as it relates to your individual situation. Be aware that some feline diseases, such as feline herpesvirus or panleukopenia, do not need direct contact with infected animals, and can spread to indoor cats.
That said, the decision to vaccinate, even with core vaccines, should depend on a professional assessment of the risks for each cat, and each vaccine. For this reason, we strongly recommend having a discussion with your veterinarian before deciding what is right for your cat.

Conclusion
Although rare, feline injection-site sarcomas are a recognized risk associated with vaccination. The exact cause is still unknown, but numerous studies suggest that adjuvant vaccines may induce an inflammatory reaction at the injection site, contributing to the development of sarcomas.
Since the discovery of this condition, there have been alterations made to feline vaccination guidelines to aid in the management and avoidance of injection site sarcomas, including the recommended location for injections, and the development of non-adjuvant vaccines.
The low risk of FISS does not justify avoiding vaccinating your cat, but it is a factor you may wish to discuss with your veterinarian. They have the expertise to help you make an informed decision about what will be the best option for your beloved feline companion.
Featured Image Credit: Dina da, Shutterstock