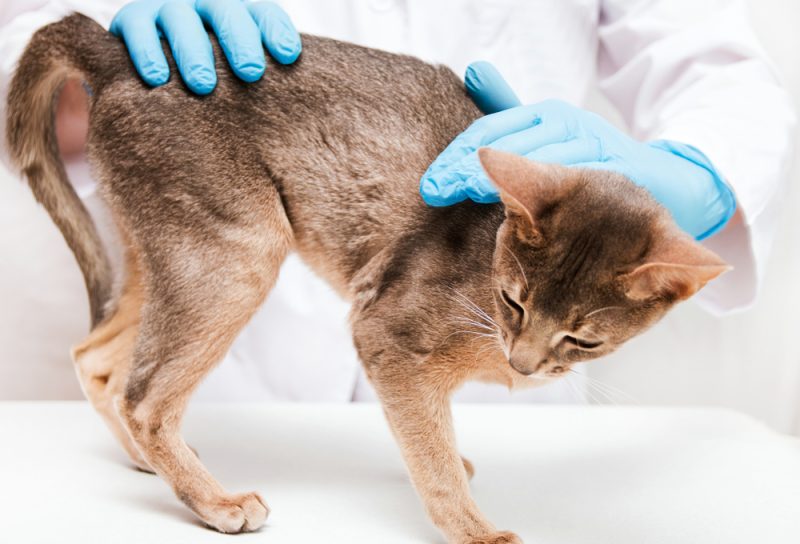
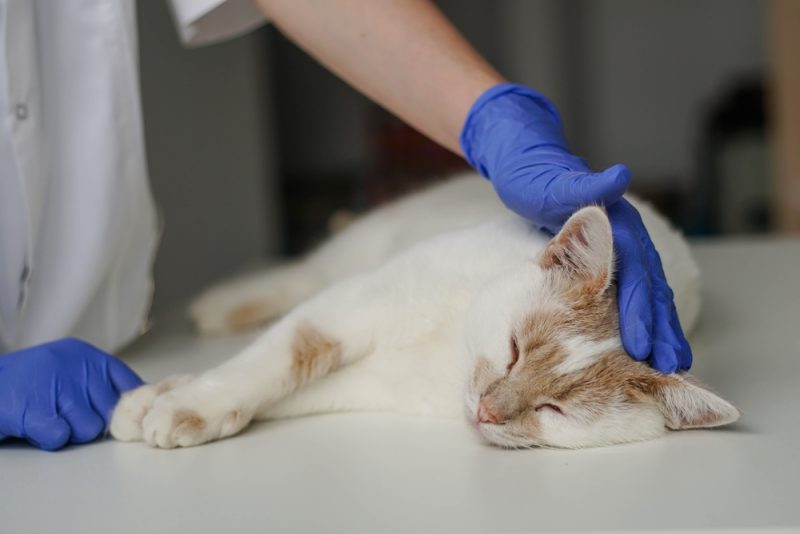
If you are a dog owner, there’s a good chance you’ve heard of Cushing’s disease. If you are owned by a cat, however, you might not be familiar with it, for good reason. Cushing’s disease, or hyperadrenocorticism, is a condition that almost exclusively affects dogs, most commonly in Miniature Poodles, Dachshunds, Boxers, and Yorkshire Terriers. Most vets will never see a case of feline Cushing’s disease, but they can—and do—occur.
Before we delve too deeply into the specifics of Cushing’s disease in cats, let’s familiarize ourselves with the basics. In order to understand what hyperadrenocorticism is, we need to know some simple anatomy and how the stress response system works.

The Hypothalamic-Pituitary-Adrenal Axis: A Simplified Version
Cushing’s disease is a complex disorder involving key endocrine (hormonal) pathways and has a knock-on effect on virtually all other organ systems.
- Cortisol: A steroid hormone produced by the adrenal glands that modulates the body’s response to physiological stress.
- The adrenal glands: Tiny, peanut-shaped structures that sit just in front of the kidneys (left and right).
- The hypothalamus: Sits in the base of the forebrain and controls the autonomic nervous system and pituitary gland1.
- The pituitary gland: A tiny gland at the base of the brain that controls endocrine function.
All these components follow a negative feedback system2.
As cortisol levels in the blood drop, the hypothalamus tells the pituitary gland to produce ACTH (adrenocorticotropic hormone), which tells the adrenal glands to produce more cortisol. Once cortisol levels are at the appropriate level, the hypothalamus tells the pituitary gland to stop producing ACTH, which tells the adrenal glands to halt cortisol production.
There are a number of ways in which this system can go wrong, and one of them results in the excessive production of cortisol—hyperadrenocorticism, also known as Cushing’s disease.
What Is Cushing’s Disease?
Named after Harvey Cushing3, the pioneering neurosurgeon who first described the disorder, Cushing’s disease is the result of an excess of the hormone cortisol being produced by one or both adrenal glands.
- A functional pituitary adenoma: This is a benign tumor that causes the pituitary gland to ignore the hypothalamus and continue to produce ACTH, which stimulates both adrenal glands to produce more cortisol despite rising levels in the blood. This is known as Pituitary-Dependent Hyperadrenocorticism (PDH).
- A functional adrenal adenoma (benign) or adenocarcinoma (malignant): In this situation, the adrenal gland with the tumor keeps producing more cortisol despite the lack of ACTH from the pituitary gland, also known as adrenal-dependent hyperadrenocorticism (ADH).
There is a third presentation of hyperadrenocorticism: Iatrogenic Hyperadrenocorticism. This occurs when animals being treated with corticosteroids (e.g., prednisone) develop the clinical signs of Cushing’s disease. However, this is also extremely rare in cats.

What Are the Signs of Cushing’s Disease in Cats?
The signs of Cushing’s disease in cats are similar to those seen in dogs and include:
- Polyuria (increased urination) and Polydipsia (increased thirst)
- Pot-bellied appearance
- Thin, fragile skin
- Poor coat quality and thinning hair
- Increased appetite
- Lethargy
- Respiratory infections
- Skin infections
- Comedones (blackheads)
- Enlarged liver
Many of the signs listed may also be seen with a number of more common conditions in older cats, such as diabetes, kidney disease, and hyperthyroidism, which would need to be ruled out. If you would feel concerned for your cat’s health, the best thing you can do is consulting your vet.
If you need to speak with a vet but can't get to one, head over to PangoVet. It's an online service where you can talk to a vet online and get the advice you need for your pet — all at an affordable price!

How Is Cushing’s Disease Diagnosed?
As a relatively common disease in dogs, canine Cushing’s disease is usually suspected based on the history, clinical signs, and breed of the patient and is confirmed with blood tests. However, Cushing’s disease in cats usually affects female cats of any breed older than 10 years. The most consistent and prominent clinical sign is their thin, fragile skin, which often suffers damage from the blood tests necessary to make a diagnosis.
These cases are further complicated by the fact that they often have concurrent, insulin-resistant diabetes, culminating in a fairly unhappy feline patient whose worsening clinical signs, coupled with the likely reluctance of their owners to submit to repeated blood tests, make diagnosis extremely challenging.
The initial workup of these cases involves routine biochemistry and hematology evaluations, which, when paired with clinical signs, would lead to further investigations. The laboratory findings in feline Cushing’s disease patients differ markedly from the results seen in dogs.
In canine hyperadrenocorticism, the effects of cortisol lead to significantly elevated liver enzymes, which are a strong indicator of the condition. In cats, the hematology and biochemistry are largely consistent with a diabetic patient, as cortisol does not cause the same increases in liver parameters, making diagnosis even more difficult, and clinical signs tend to be the main driver behind more targeted testing.
The tests required to diagnose Cushing’s disease involve artificially manipulating the Hypothalamic-Pituitary-Adrenal Axis, using either:
Low-Dose Dexamethasone Suppression Test
This involves measuring the cortisol levels in the blood following the administration of a synthetic steroid hormone, dexamethasone. In a non-Cushing’s patient, this should trigger the negative feedback system to result in a lowering of blood cortisol, whereas a patient with hyperadrenocorticism will either show no or partial suppression of cortisol levels.
In cats, the amount of dexamethasone needed to create the suppression response is significantly higher than in dogs, and their patterns of suppression tend to vary more than their canine counterparts.
ACTH Stimulation Test
As the name suggests, cortisol levels are measured before and after a synthetic ACTH analog is injected. In normal animals, the post-stimulation cortisol levels should remain within the normal range due to the negative feedback system. Elevated cortisol levels following ACTH stimulation are diagnostic for hyperadrenocorticism in dogs, but in cats, this test often gives false negatives.
Urinalysis to assess urine concentration and cortisol levels may also be used to help diagnose feline Cushing’s patients. Imaging such as ultrasound, CT, or MRI may also be utilized in cases where a diagnosis has not yet been established.
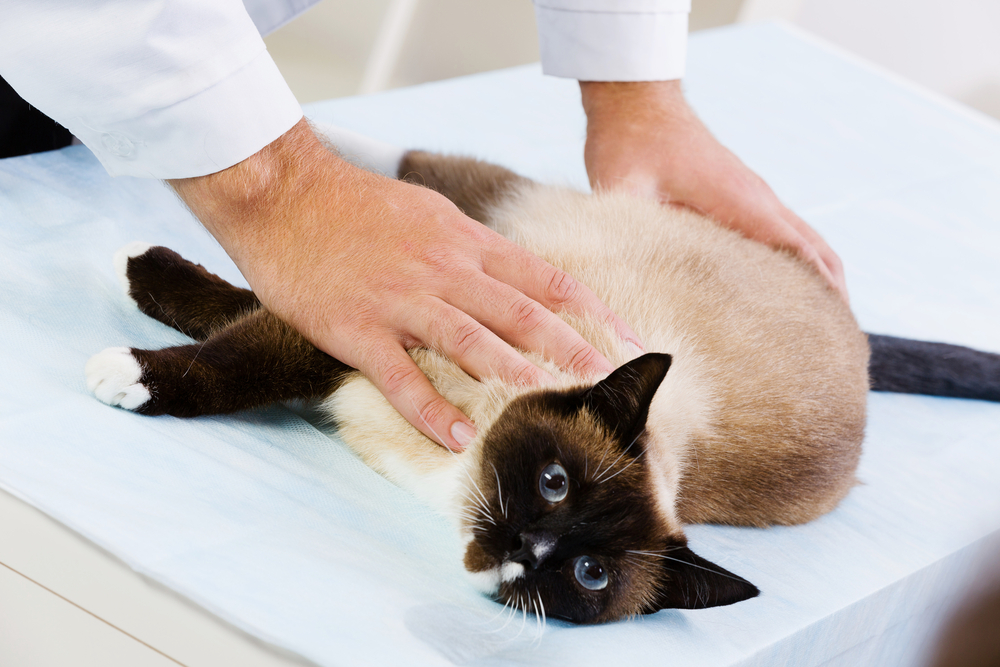
How Is Cushing’s Disease in Cats Treated?
Due to the high level of surgical complication and mortality in dogs, treatment for canine hyperadrenocorticism is almost always medical. Mitotane, a cytotoxic drug that targets adrenal tissue, or Trilostane, an adrenal enzyme inhibitor, are the mainstays of treatment in dogs. However, neither drug has a substantial amount of information regarding safety or effectiveness in feline cases, but both are still used in clinical practice.
Studies indicate that cats have a much lower postoperative complication rate than dogs, making adrenalectomy a more viable option. Radiation therapy for PDH patients is also an option, though a rarely used one.
The prognosis of these cases will depend greatly on how well they respond to treatment, as well as concurrent illness. Ultimately, Cushing’s disease will shorten life expectancy to anywhere from several months to 2–3 years following diagnosis.

Conclusion
Cushing’s disease is a rare condition in cats; however, given the difficulty in diagnosing and treating it, it is possible that there are more cases that go undiagnosed. It certainly wouldn’t be high on many lists of differential diagnoses. One of the greatest challenges in identifying feline cases is the fact that many of the clinical signs and initial blood results are consistent with unresponsive diabetes, which may be occurring at the same time. Coupled with their inconsistent response to more specific diagnostic testing, it is remarkable that cases are successfully diagnosed at all.
Although the disease shares most of the fundamental characteristics of canine hyperadrenocorticism, cats do not respond with the same level of predictability during diagnostic workups and are more limited in terms of treatment options and, therefore, prognosis.
The most common clinical signs of Cushing’s disease are PU/PD, lethargy, weight loss or altered weight distribution, increased appetite, and poor skin and coat conditions. These can also accompany a number of diseases in older cats, all of which require veterinary attention. If any of these changes are affecting your cat, a veterinary examination is needed.
Featured Image Credit: Nataly Mayak, Shutterstock