As exciting as it is to bring home a new cat to join your family, the experience can also be somewhat stressful, and you’ll want to make sure you have everything you need to ensure your feline (and you) are as comfortable as possible. There are essential items to have at the ready, beyond the basics like bedding and food, and there are other important factors to consider too.
By preparing thoroughly in advance, you can make your new cat’s transition into their new home as smooth as possible. Making sure your new cat has all the essentials and a proper introduction to your family and other pets will help ensure that everything is in order before the big day.
If you are adopting a new feline, you’ve come to the right place. We’ve created this adoption checklist with all the essentials that you need to purchase, tips on preparing your home, and pointers on how to introduce your cat to your family and pets to make the process as smooth as possible for all involved.
Essential Supplies for Your Cat Adoption
As with any pet, there are a few supplies to purchase to make sure your new cat is comfortable. The following are the basics to have before bringing home your new cat.
The views and opinions expressed are not necessarily those of the veterinarian. We recommend contacting your veterinarian before purchasing any product from this list.
1. Bed and Bedding

Your cat will need somewhere comfortable to sleep and feel safe. Although cats will often sample and try a few different beds before settling on a favorite, it’s still a good idea to have at least one available when you first bring them home. Your cat’s bed is more than just a place to sleep; it can also be a safe sanctuary for them to have alone time and can become a place associated with comfort and safety. Cat beds come in a wide variety of shapes and sizes, from basic sleeping mats to safe and luxurious cat caves and elevated beds.
Keeping your cat comfortable and feeling secure when you are away will have them well rested and ready to play when you return. The Hepper Nest is a modern cat bed designed to meet the specific needs of cats. Its high sides offer a sense of security and the bowl shape gives support like a warm hug from their favorite person. Learn more about why your cat will thrive in your absense with the Hepper Nest by clicking here.
At Catster, we’ve admired Hepper for many years and decided to take a controlling ownership interest so that we could benefit from the outstanding designs of this cool cat company!
2. Food and water bowls

Your cat will need separate food and water bowls, preferably made from ceramic or stainless steel. Cat bowls can be as simple as you like, but there are unique options available too. Cats are often drawn to a , as flowing water tends to pique their curiosity. There are also great automated feeders that may help with feeding your cat a small portion of food while you’re away. Of course, make sure you have good-quality food on hand too.
- NO MESS - The 360° tray on this cat food and water bowl set has a raised design to catch and...
- WHISKER FRIENDLY - Shallow and wide metal containers with flat bottoms ensure your kitty can enjoy...
- CHEW-SAFE MATERIALS - Kittens and cats love chewing on silicone and soft rubber - but it's a choking...
Choosing the right food and water bowls for our feline companions can pose certain challenges for pet owners. The Hepper NomNom Cat Bowl provides a chic and innovative solution that supports cat specific needs, such as shallow bowls and a subtle elevation that fosters whisker relief, posture comfort, and improves digestion. It features an elegant contemporary design with a wide wrap-around tray aimed at minimizing any messes from ending up on your floor! Furthermore, this bowl is entirely dishwasher safe, so pet owners are able to spend more time with their cats instead of cleaning up after them. Discover why the Hepper NomNom Cat Bowl is right for both you and your kitty by clicking here.
At Catster, we’ve admired Hepper for many years and decided to take a controlling ownership interest so that we could benefit from the outstanding designs of this cool cat company!
3. Litter tray

A litter tray or box is an important item for any cat, but new cats in particular will not be going outside and need a place to safely do their personal business. There are a ton of different types of boxes and litter available, from the trays to automated self-cleaning versions. We recommend a large box, as cats like to turn around and dig in them, and even if you only have one cat, we recommend having at least two trays for them. The total number of litter boxes that you should have at a minimum is one more than the number of cats that you have.
4. Scratching Post

Toys are an essential item when bringing home a new cat. They will keep your cat physically and mentally stimulated and provide a fun way to bond with your feline. There are an infinite amount of toys available, from basic ball toys to complex electronic toys.
We're quite fond of cardboard as a material in cat scratchers, which is why we love the Hepper Hi-Lo Cat Scratcher. Encased within a well-constructed, modern birch plywood frame, this scratcher is designed with both cats and their owners in mind. It offers three versatile configurations to keep your feline friend active and entertained while enticing them to fulfill their natural scratching instincts (and away from scratching things they shouldn't). For more details, click here! At Catster, we’ve admired Hepper for many years, and decided to take a controlling ownership interest, so that we could benefit from the outstanding designs of this cool cat company!
5. Toys

Toys are an essential item when bringing home a new cat. They will keep your cat physically and mentally stimulated and provide a fun way to bond with your feline. There are an infinite amount of toys available, from the basic ball toys to complex electronic chasing toys and of course, the classic laser pointer.
Our Favorite Cat Toys Right Now Here are a some of our favorite toys, each catering to a variety of senses and play preferences. Which one will your feline fancy? At Catster, we've admired Hepper for many years, and decided to take a controlling ownership interest so that we could benefit from the outstanding designs of this cool cat company!
Image
Product
Details

Hepper Catnip Mice Toy Set
Check Price

Hepper Furball Set
Check Price
6. Microchip
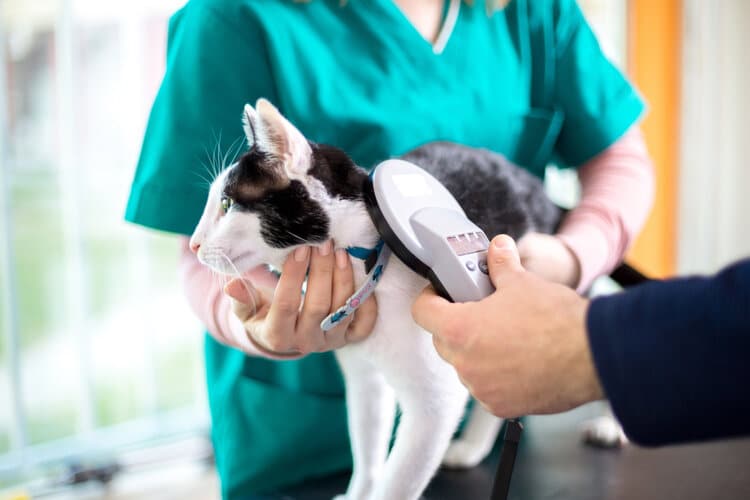
Most cats that are adopted from shelters should be microchipped, and if your cat has not yet been microchipped, we highly recommend getting the procedure done. This will help you find your cat should they get lost and will hold all their important information. A cat collar with tags is also a great idea and is a quick and simple way to identify your feline. It’s best to ensure that your cat’s collar is a breakaway type, as this offers additional safety for your cat should it ever snag onto something.
7. Grooming Equipment

It’s important to give your cat regular brushing, especially breeds like Persians that have long coats, to prevent knotting and matting. The brush that you buy will largely depend on the breed of cat that you adopt and their coat type.
If you are looking for recommendations on the best cat brush, you should check out Hepper Cat Brush. You will hardly find different brush with so many pros - easy to clean, easy to use, durable and effective. Simply everything you need from a cat brush. Click here to order yours today.
8. Travel Crate

A crate or carrier is an important item to bring home your new cat from the shelter or breeder and will be essential for vet visits too.

Preparing Your Home
With these essentials ready, you should be able to move forward with preparing your house for your new pet.
If You Have Other Pets
As a health precaution, always quarantine a new pet away from your existing pets for a period of at least 2 weeks. During this time, ensure that you don’t share bowls, litter boxes, toys, beds, and other tools (e.g., nail clippers) among your cat and your existing pets. Thoroughly wash your hands before and after you interact with each one of your pets.
The new addition to your family might be harboring an illness that could spread to your existing pets if you rush an introduction. A period of at least 2 weeks gives you enough time to observe the newcomer to see if they develop signs of an illness.
Ensure that your veterinarian gives your new pet a thorough checkup before attempting a physical introduction with your existing pets. It is ideal to have a new cat examined by your veterinarian both at the start and end of their quarantine period.
If you need to speak with a vet but can't get to one, head over to PangoVet. It's an online service where you can talk to a vet online and get the advice you need for your pet — all at an affordable price!

If You Don’t Have Other Pets
Ensure that your cat will have a safe, quiet, and comfortable place where they can be by themselves. Introduce them to this area first, and try to keep them there for a day or two. Keeping them in a comfortable confined space will help prevent them from getting overwhelmed by their new environment, and they can slowly get to know you too.
Make sure they have food, water, and their litter box close by, along with their bed or travel crate and toys. Cats are curious animals, so you’ll need to make sure that there are no breakables, like glass vases, around and that the area is free from electrical cords and wires.
Once you feel like your cat is comfortable, you can start to introduce them to the rest of your home. We recommend just leaving the door open and letting your cat explore in their own time and at their own pace; you should never rush this process.

Final Thoughts
Bringing home a new cat is an exciting time, but it can also be stressful if you are a first-time cat owner. By making sure that you have all the necessary items and that your home is ready, you can reduce this stress enormously and focus on the excitement and fun of getting to know your new feline friend.
Featured Image Credit: Andriy Blokhin, Shutterstock














