World Rabies Day is an international awareness campaign occurring on September 28th annually.
Though rabies may not often be talked about in places like the U.S. and Canada, thanks to high vaccination levels in domesticated pets, it remains a significant health problem in countries worldwide. The fact remains that rabies is 100% preventable, yet nearly 60,000 people die from it every year.
Read on to learn more about World Rabies Days and what is being done to raise awareness.
What Is Rabies?
Rabies is a 100% preventable viral disease that can be transmitted via the bite or scratch of a rabid animal. The virus affects the central nervous system, causing disease in the brain and eventually death.
- Furious rabies (noted by hyperactivity and hallucinations)
- Paralytic rabies (noted by paralysis and coma)
Rabies is almost 100% fatal once clinical signs begin.
Most cases reported to the Centers for Disease Control and Prevention occur in wild animals, though any mammal can contract the disease. While the tens of thousands of rabies cases that arise in humans annually, almost all of them are acquired from the bite of an infected dog.
However, a cat with rabies can be passed to their owners or anyone the cat bites. Signs your cat might have rabies include:
- Changes in behavior
- Becoming aggressive
- Inability to swallow; drooling
- Decrease in muscle control
Rabies may not often be talked about in places like the U.S. and Canada due to high vaccination levels in domesticated pets; however, it remains a significant health problem in countries worldwide. Though rabies is a 100% preventable disease, nearly 60,000 people (mostly children) die from rabies globally every year.

What Is World Rabies Day?
World Rabies Day is celebrated to raise awareness about the prevention of this horrible disease as well as to highlight the progress made in defeating it.
September 28th was chosen as World Rabies Day as it is the date Louis Pasteur died. Pasteur was a French chemist and microbiologist who, along with his colleagues, developed the first rabies vaccine.
Every year, the Rabies Alliance chooses a theme that they believe is relevant to the current rabies situation and global trends relating to the disease.
What Is Being Done About Rabies?
Tremendous efforts are made across multiple sectors in the United States and Canada to prevent rabies. Wildlife biologists distribute millions of rabies vaccine baits to wild animals to stop virus transmission at its source. Veterinarians vaccinate over 40 million domesticated cats and dogs annually to provide disease protection for the animals and their families. Humane societies and rescues provide shelter to stray animals, giving them a home off of the streets and reducing the spread of the virus. Scientists work diligently to develop new prevention methods, including new vaccines and treatment modalities.
The World Health Organization has a global strategic plan to end human deaths from dog-mediated rabies by 2030. This plan, “Zero By 30”, consists of a three-phase approach to engage, empower, and enable countries to focus on elimination efforts.
- Effectively using vaccines, medicines, tools, and technologies to reduce human rabies risk.
- Generating and measuring the impact of the efforts by ensuring reliable data and implementing effective policies.
- Sustaining commitment and resources by harnessing multi-stakeholder engagement.
What Can I Do to Celebrate World Rabies Day?
There are many things you can do to acknowledge World Rabies Day.
- Spread the word. Because rabies isn’t as prevalent in Canada and the United States as it is in other places around the world, the best thing you can do on World Rabies Day is spread awareness about this horrifying disease.
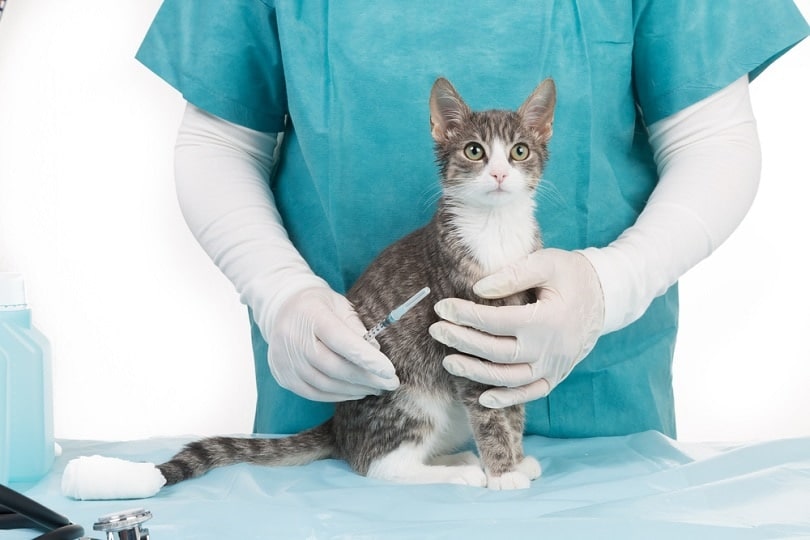
- Promote vaccination. Vaccination against rabies is one of the best ways to prevent the transmission of the disease. If your pets have not had their rabies vaccines or their booster shots, it’s time to contact your vet and have them inoculated. Cats and dogs require a booster one year after their first rabies vaccine and boosters every 3 years thereafter. Depending on the laws where you live and the vaccine used, your pets may need boosters annually versus every 3 years.
- Educate yourself on bite prevention. Bite prevention is key in reducing your risk of contracting the disease. Leave all wildlife alone and know your risk; most cases of rabies deaths in the U.S. occur through contact with infected bites, followed by exposure to rabid dogs whilst traveling internationally.
- Spay and neuter your pets. Spaying and neutering reduces the number of unwanted pets that either become strays or are improperly cared for or regularly vaccinated.
Rabies By the Numbers
According to statistics released by the World Health Organization and the CDC during last September’s World Rabies Day celebration:
- About 4 million Americans are bitten by animals each year.
- Close to 800,000 of those Americans received medical attention for these bites.
- Approximately 60,000 Americans are estimated to have been exposed to the rabies virus and receive treatment for it.
- Less than 4,000 animals test positive for the virus, mostly rats, skunks, foxes, cats, and dogs.
- Only 241 cases of rabies were reported by the CDC in 2018.
- Less than 3 rabies deaths in the United States.
- 95% decline in human deaths from the peak in 1945.
- Rabies accounts for 59,000 human deaths in over 150 countries.
- 95% of rabies cases occur in Africa and Asia.
- Half of rabies cases occur in children under 15 years of age.
Final Thoughts
Rabies is a horrifying disease that results in tens of thousands of deaths annually. Much has been done about the disease over the last several decades, and though the number of cases reported every year is dwindling, more needs to be done to achieve zero cases by the year 2030.
By celebrating World Rabies Day every year, we can promote awareness about this awful disease and do our part in achieving a rabies-free world.
Featured Image Credit: elwynn, Shutterstock












